Understanding Graves’ Disease: Symptoms, Causes & Treatment
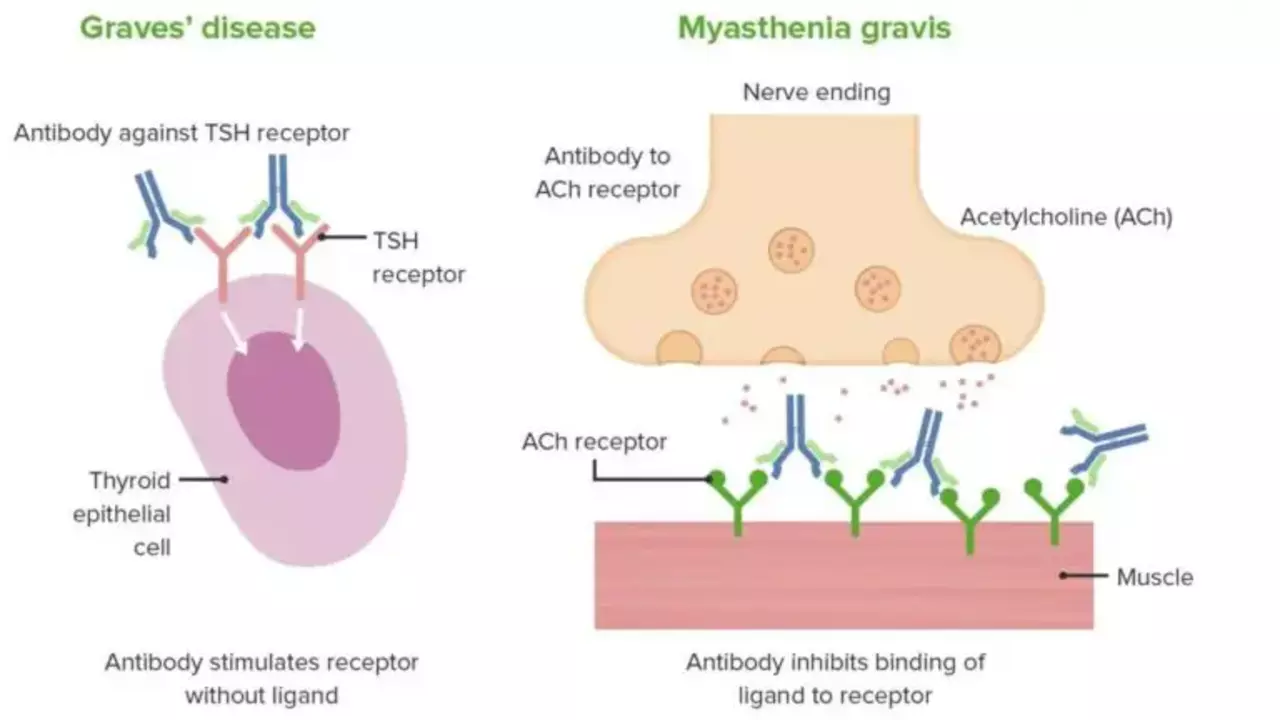
If you’ve heard the term "Graves’ disease" and felt a bit lost, you’re not alone. It’s basically an autoimmune form of hyperthyroidism where your body tricks the thyroid into making too much hormone. Too much thyroid hormone speeds up almost everything in your body—heart rate, metabolism, even mood. The good news? Knowing the signs early can save you from uncomfortable surprises and give you a clear path to feel better.
Common Symptoms & Warning Signs
Most people notice a rapid heartbeat or palpitations first. You might also feel shaky hands, heat intolerance, or sudden weight loss despite eating normally. Eye changes are a hallmark—eyes can look protruding (called exophthalmos) or feel dry and gritty. Some report anxiety, irritability, or trouble sleeping because the nervous system is on overdrive. If you’ve experienced any of these for weeks on end, it’s worth getting thyroid labs checked.
How to Manage and Treat Graves’ Disease
Treatment starts with confirming the diagnosis—blood tests for TSH, free T4, and antibodies, plus a neck ultrasound if needed. Doctors usually recommend one of three routes: antithyroid meds (like methimazole) that block hormone production, radioactive iodine to shrink the thyroid, or surgery to remove part of it. Each has pros and side‑effects; for example, medication is quick but needs regular monitoring, while radioiodine can cause temporary worsening of eye symptoms.
Beyond medical options, lifestyle tweaks help a lot. Limit caffeine and sugary foods that can aggravate jitteriness. A balanced diet rich in calcium and vitamin D supports bone health, which can be at risk with high thyroid levels. Gentle exercise—walking, yoga, or swimming—helps control weight and reduces stress without overtaxing the heart.
If eye problems are a big concern, an ophthalmologist may suggest steroids or special eye drops to reduce inflammation. Some patients also benefit from beta‑blockers (like propranolol) that calm the rapid heartbeat while other treatments take effect.
Regular follow‑ups are key because Graves’ disease can shift—sometimes it goes into remission on its own, and sometimes hormone levels swing back up after treatment. Keeping a symptom journal makes those appointments more productive; note any changes in energy, mood, or eye appearance.
Bottom line: Graves’ disease is manageable once you recognize the signs and work with a healthcare team that tailors therapy to your needs. Early testing, a clear treatment plan, and supportive habits can get you back to feeling like yourself again.
Graves' Disease and Pregnancy: What You Need to Know
In my latest blog post, I delve into the topic of Graves' disease and its implications for pregnancy. I've discovered that this autoimmune disorder can complicate pregnancy if not properly managed, with effects on both the mother and baby. It's key for women with Graves' disease to work closely with their healthcare providers before and during pregnancy to minimize these risks. Treatment options do exist and include medication, surgery, or radioactive iodine therapy. Despite the challenges, many women with Graves' disease have successful pregnancies with the right care and management.